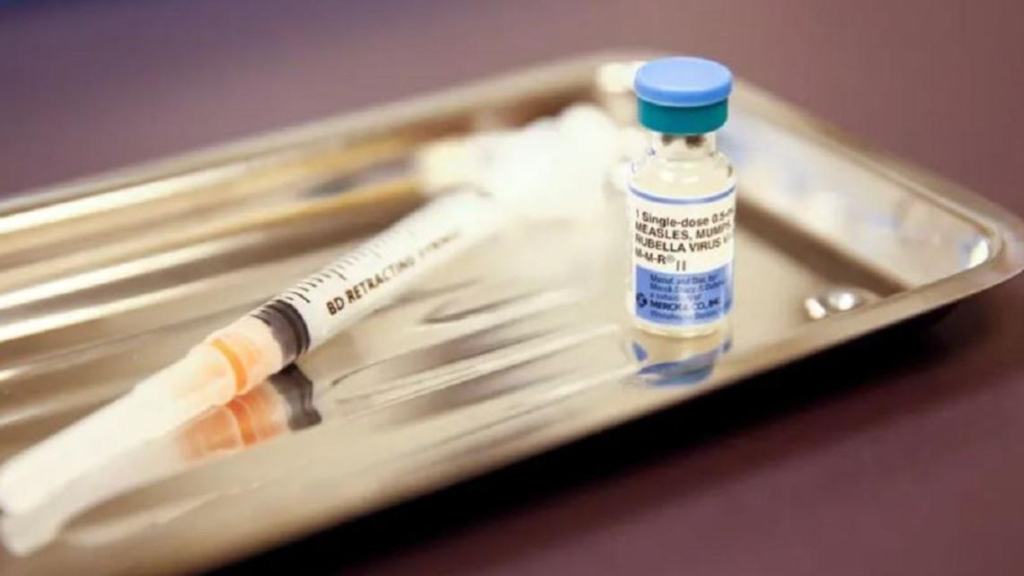
Five years ago, Melanie Richburg used a roll of duct tape, a HEPA filter, and a portable fan to create a makeshift air filtration system in a hospital room where COVID-19 patients were being tested.
Now, as the largest measles outbreak in Texas in three decades spreads in the South Plains region, the Lynn County Hospital District—where Richburg serves as CEO—still lacks specialized isolation rooms for patients.
Once again, she’s prepared to use duct tape if necessary.
“If the number of patients surpasses the available beds at children’s hospitals, we’ll need a backup plan,” said Richburg, whose county is located 30 miles south of Lubbock and has reported two measles cases. “The challenge we’re facing now is the same one we had during COVID.”
The coronavirus pandemic highlighted the crucial need for strong public health infrastructure and revealed the stark divide in health services between urban and rural areas. In the aftermath, federal funding flowed to local health districts, and policies to address healthcare deserts gained traction.
Yet, as measles, a disease that was declared eliminated in the U.S. in 2000, resurges, rural West Texas communities and state officials are scrambling to respond. Aging infrastructure, a shortage of primary care providers, and long distances between testing sites and labs are major hurdles, especially in rural areas like those impacted by the measles outbreak.
Since late January, at least 198 Texans have contracted measles, and one child has died—the first measles-related death in the U.S. in a decade. More cases are anticipated, and the outbreak may last for months, according to state health services commissioner Jennifer Shuford.
Though measles differs from COVID-19 in many ways, it’s similarly exposing how the lack of public health resources leaves rural communities vulnerable. Local leaders are forced to make do with limited tools, all while dealing with years of inadequate investment from state and federal governments in proactive health measures.
“We’re in a public health shortage area,” said Gordon Mattimoe, director of the Andrews County Health Department. “You have to think outside the box.”
A Lack of Infrastructure Around 64 counties in Texas have no hospital, and 25 counties lack primary care physicians, according to the Texas Department of Agriculture. Between 2010 and 2020, 26 rural hospitals in the state closed, according to a rural hospital trade group. Although the pace of closures has slowed since then, many remaining hospitals are in dilapidated buildings with a limited number of medical staff.
Large areas of Texas also lack public health campaigns to educate residents, and the shortage of medical staff makes it harder to provide individual education on vaccination and regular health visits.
“We have a hard time finding pediatricians for newborns,” said Sara Safarzadeh Amiri, chief medical officer for Odessa Regional Medical Center and Scenic Mountain Medical Center. “That’s a problem. If there’s a serious health issue, who do you ask?”
Most measles cases in Texas are among unvaccinated school-aged children, and the outbreak is particularly concentrated in the Mennonite community in Gaines County. Cases have also been reported in eight other counties, from Dallam near the Oklahoma border to Ector, south of Gaines.
To contain the disease, rural health teams have set up makeshift testing spaces, used social media to spread vaccination information, and driven specimens across counties to be tested at the only state lab in Austin. Last week, Texas Tech University’s Bioterrorism Response Laboratory, part of a national network of CDC-funded labs, began processing measles tests.
Testing is vital for measles, experts say, because individuals infected with the disease can spread it for several days before symptoms show. They must isolate to prevent further transmission.
In Gaines County, runners have had to drive specimens up to 70 miles to a FedEx office, where they are then shipped to the state lab. It can take up to 48 hours to get test results. During that waiting period, public health officials ask patients to quarantine, but they can’t be sure they will comply.
“Some people need to see the test results before they take action or follow quarantine instructions,” Amiri said. “Having testing available is crucial.”
In nearby Andrews County, Mattimoe is using the old City Hall as a testing site because he doesn’t have a reverse pressure room—a specialized area recommended by the CDC to isolate contagious patients. Without such a room, rural counties like Lynn and Yoakum have improvised measles testing areas, hoping they can manage the flow of patients.
Mattimoe opted for the City Hall space, as it is vacant, and without it, he’d have to shut down the entire department for two hours between cases.
Reactive, Not Proactive Public health efforts are meant to focus on prevention, yet emergencies often spur the most significant action, especially in rural areas.
The outbreak only intensified when a child died from measles. In response, state and federal support increased. Last week, 27 contractors were sent to the outbreak zone, a public awareness campaign with billboards and social media ads was launched, and CDC disease detectives were deployed.
Local officials also ramped up efforts. In Ector County, County Judge Dustin Fawcett made media appearances promoting the MMRV vaccine, which provides 97% protection against measles with two doses. The county also bought a $7,695 freezer to store measles test specimens, which must be kept at -70°C.
In Andrews County, Mattimoe saw a surge in people getting vaccinated after the death of a child. “Sadly, that tragedy brought many people in to get vaccinated,” he said.
Despite increased state and federal efforts, experts argue that vaccination campaigns should have started earlier, as vaccination rates had already been declining for years.
“We shouldn’t be doing this during an outbreak,” Amiri said. “We should have been doing it ahead of time to prevent the outbreak.”
In rural areas, getting vaccines into residents is complicated by Texas’ mostly decentralized public health system. Cities and counties have their own departments, but many rural areas can’t afford their own systems and instead rely on one of 11 regional health districts, which often lack the resources or local knowledge needed to encourage vaccination.
“You have to call small towns and find free space to set up a clinic,” said Katherine Wells, director of Lubbock’s public health department. “Then you’re driving from Lubbock to rural areas, which limits how long you can keep clinics open.”
Adding to the challenge, public health messaging is often muddled. Health and Human Services Secretary Robert F. Kennedy Jr. has downplayed the outbreak and framed vaccination as a personal choice.
“As the federal landscape shifts, it’s clear that strengthening local public health systems is essential,” Amiri said.
The Importance of Funding Years of underfunding in public health left Texas unprepared for the COVID-19 pandemic. Hospitals lacked equipment, and health departments had outdated technology that hindered data access. The pandemic exposed deep disparities between urban and rural healthcare access, with residents of counties without hospitals dying from COVID at rates 20% higher than those in counties with hospitals.
Federal funding helped alleviate some of the pressure. In 2020, Texas received $35.5 million in public health infrastructure grants, and the CDC’s five-year Public Health Infrastructure Grant is sending $221 million to the state.
These funds have enabled some rural health departments to expand and respond to the measles outbreak. For example, the Lubbock health department nearly doubled in size thanks to a $2 million grant, enabling it to ramp up testing and vaccination efforts. In Andrews County, Mattimoe has used grant money to expand his department and offer year-round vaccine clinics.
“Community immunity has really helped protect us,” Mattimoe said. “We haven’t had any measles cases so far.”
Although the funding has been vital, Texas still lags in public health spending. The state spends just $17 per person on public health, less than most other states, and down from $19 per person a decade ago.
Richburg, the CEO in Lynn County, had hoped the makeshift system she used during COVID wouldn’t be necessary again. Last year, she proposed a bond to fund infrastructure upgrades, including negative pressure rooms for isolation, but voters rejected the tax increase.
“We wanted those beds for situations where patients need isolation, not a room with a broken window and a fan duct-taped in,” she said.
Lynn County’s healthcare system is also in dire need of an electrical upgrade, as the backup generator doesn’t support essential equipment like MRI and CAT scan machines. Despite the challenges, Richburg remains determined.
“We’re still here, the lights still come on every morning, and patients still come in for services,” she said. “We’re not going away.”